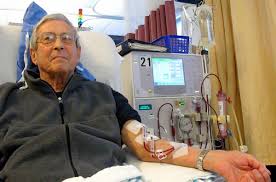
Dialysis access serves as the link between the body and the machine that performs life-sustaining blood filtration for people with kidney failure. While dialysis treatments themselves receive most of the attention, the quality and maintenance of dialysis access often determine the success of therapy. Without reliable access, the efficiency and comfort of treatment can be compromised, potentially affecting long-term health outcomes. Understanding the types of access and how they function provides a clearer picture of how they support kidney health.
Understanding Types of Access and Their Function
Three main forms of dialysis access are used for hemodialysis: arteriovenous fistulas, arteriovenous grafts, and central venous catheters. Each serves the same purpose but differs in how it is created and how well it performs over time. Arteriovenous fistulas are formed by connecting an artery directly to a vein. This causes the vein to grow stronger, making it easier to insert needles for each treatment. Fistulas are often the preferred option because they tend to last longer and have fewer complications. Arteriovenous grafts involve placing a synthetic tube between an artery and a vein. This approach is used when a fistula is not possible due to vein condition. Grafts can be ready for use sooner than fistulas but may have a higher risk of infection or clotting.
Knowing Why Access Influences Overall Treatment Success
Well-functioning dialysis access allows the machine to filter blood at an adequate rate, which helps prevent the buildup of toxins and excess fluid. If blood flow through the access is restricted, treatment becomes less effective, and symptoms such as fatigue or swelling may worsen. Access issues may also lead to treatment delays or emergency procedures, both of which can impact quality of life.
Because dialysis must be performed multiple times each week, the access site is used repeatedly. Keeping it in good condition allows for reliable therapy without complications like clotting, bleeding, or infection. Regular monitoring and routine care help detect problems early and avoid more serious disruptions.
Preventing and Maintenance Supports Access Longevity
Protecting dialysis access involves a combination of patient habits and clinical monitoring. Patients are encouraged to check their access site daily for signs of swelling, pain, or changes in pulse. Any unusual changes should be reported promptly.
Clinics use tools like ultrasound or access flow studies to monitor the site’s function. These tests identify narrowing or blockages that could restrict blood flow. If detected early, minor issues can often be treated with a simple outpatient procedure.
Avoiding pressure or injury to the access arm also helps preserve long-term function. Blood pressure should not be taken on that arm, and carrying heavy loads should be avoided. These precautions reduce stress on the vessels and minimize the risk of complications.
Planning Access Before Dialysis Begins Improves Outcomes
Whenever possible, dialysis access should be planned in advance of treatment. Early referral to a nephrologist or vascular surgeon allows time to evaluate the best type of access and schedule the necessary procedure. This proactive approach increases the likelihood of using a fistula, which generally has the best long-term outcomes.
When treatment begins without established access, temporary catheters may be used. However, the goal is often to transition to a fistula or graft as soon as possible. Early planning gives the fistula time to mature and avoids complications linked to temporary solutions.
Take the Next Step in Dialysis Access
Dialysis access may seem like a small piece of a complex process, but its role is foundational. Without healthy access, treatment cannot be delivered as intended. Whether preparing for dialysis or currently receiving it, staying informed and proactive about access care helps maintain comfort, reduce risks, and improve outcomes. For anyone managing kidney disease, discussing access options early and following through with proper care creates a stronger path toward long-term health.
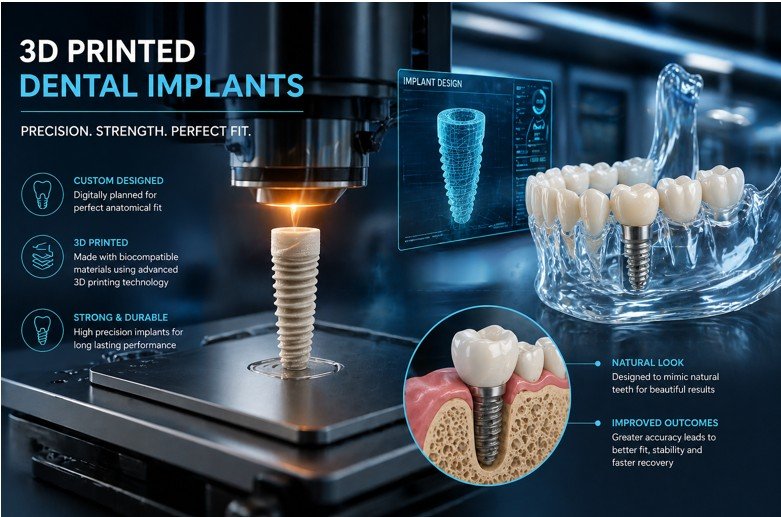
- The Future of Tooth Replacement: Exploring 3D Printed Dental Implants
- A Deep Dive into the TRIOS 6 Wireless Intra-Oral Scanner and Clinical Benefits
- The science-backed daily habits that support healthy longevity
- How Laser Hair Removal Can Simplify Your Beauty Routine
- Exploring Alternative Therapies for Back Pain



Leave a Reply